ANATOMY AND PHYSIOLIGY OF ANORECTUM.
HYPOTHESIS OF THE CONTINENCE AND DEFECATION
Levin Michael, MD, PhD, DSc,
Radiologist
State Geriatric Center, Netanya, Israel.
Amnon ve-Tamar 1/2, 42202, Netanya, Israel.
Tel: 972-53-8281-393, Fax: 972-9-8630151.
Abbreviations: ARM –anorectal malformations; IAS – internal anal sphincter; EAS – external anal sphincter; PRM – puborectalis muscle; CSS – colosigmoid sphincter; RSS – rectosigmoid sphincter; BRP – basal rectal pressure when a rectum empty or relaxed; TLP–1, first threshold level pressure which stimulates of rectoanal inhibitory reflex; TLP-2, second threshold level pressure in which appears the urge to defecate; TLP-3, third threshold level pressure for act defecation; RND - roentgen negative distance.
Objective: to clarify the normal physiology of the continence and defecation.
Material & methods
The study includes the survey of 65 children aged from 5 days to 14 years and 23 patients aged from 23 to 84 years with the normal function of the anorectum. The special modification of the barium enema was done. The radiopaque marker is located near the anus. The length of the anal canal on the lateral radiograph was measured as distance between barium in the rectum and the marker. It has allowed to evaluate the function of the puborectalis muscle (PRM). Manometric study in 32 patients was carried out including 10 children where an anal pressure was measured during the barium enema.
Results & Conclusions. On the basis of the literature data and our own research the hypothesis of the continence and defecation was proposed. It was established four levels of rectal pressure, which determines the function of the anorectal muscles. Basal rectal pressure (BRP) is defined in an empty rectum and it is equal to intra-abdominal pressure. When some fecal portion enters into the rectum and the rectal pressure rises to the first threshold level pressure (TLP-1) the relaxation of the internal anal sphincter (IAS) and contraction of the external anal sphincter (EAS) and PRM occurs (inhibitory reaction). The rectum is adapted to the new fecal volume and relaxes. The rectal pressure falls below the TLP-1 to BRP, what leads to the contraction of the IAS and relaxation of the PRM and EAS (adaptation reaction). A new fecal portion causes of the inhibitory reaction, which is replaced by the adaptation reaction. Changing the inhibitory reaction by the adaptation reaction and vice versa promotes the long-term continence. When a certain amount of stool stretches the rectal wall, the rectal pressure rises to a second threshold level (TLP-2) and a need to defecate appears. Continuous contraction of the IAS is due to the fact, that different groups of the muscle fibers are at different stages of recovery of the contractile capacity. The rectal pressure is dependent not only on the amount of the feces, but also the tone of the rectal wall.
Defecation reflex occurs at a higher rectal pressure (TLP-3), which appears during contraction of the abdominal wall and causes a reflex of the strong rectal peristalsis which expels feces. It accompanied by a contraction of the levator ani muscle, which opens the anal canal to facilitate the passage of a stool.
Key words: Physiology, rectum, anal canal, continence, defecation, anorectal sphincters, hypothesis.
Introduction
Continence and defecation are two essential functions of the human body. Continence is the ability to retain feces until an acceptable time for defecation. Defecation is the evacuation of fecal material from the colon. Both functions involve complex physiologic processes that are not completely understood [1]. Normal anatomy of the gastrointestinal tract is well documented in the literature. The data on the physiology of these processes are controversial. For example, muscular contraction is accompanied by energy expenditure and resource depletion. All of the known muscles, including the heart, relax after the contraction. During the relaxation, their contractile capacity is recovered. It is still not clear how the anal canal is in the continuous contraction, and which muscles are involved in the act of the defecation. It is known that the external anal sphincter (EAS) is responsible for the emergency continence during the increase of the abdominal pressure. However, the intensity of contraction promptly decreases after one minute [2, 3]. It is hard to ascribe the continence to continuous contraction of the internal anal sphincter (IAC).
Clear understanding of the normal physiology of the anorectal zone, could significantly improve our approach to such pathological conditions like chronic constipation, fecal incontinence, anorectal malformations, etc.
At this work presents a new hypothesis of the continence and defecation, based on the previously published researches.
Background: The digestive tract is a self-regulating system. The status of the rectum and anal canal is correlated with other parts of this system. In healthy volunteers, in response to dilatation of the esophagus at the level of the lower esophageal sphincter, a significant increase of the rectal pressure was shown. At the same time, there was no appreciable change in pressure at the level of the anal canal. Shafik has suggested that this reaction is conducted through the mesenteric plexus from the esophagus down along the gut wall to the rectum, initiating rectal contractions. It is likely that these signals the entrance of additional contents from the gut is coming - so that the rectum could evacuate its contents. [4]. At 80 ml distension, the rectal pressure rose (p < 0.001) and the balloon was dispelled to the exterior. Meanwhile, the pressure in the esophagus, corpus of the stomach and pyloric antrum showed a significant drop (p < 0.05) and in the lower esophageal sphincter and pyloric sphincter a significant rise (p < 0.05). There was no esophageal or gastric response to distension of the anesthetized rectum. Impacted feces in the rectum caused a deceleration of gastric emptying [5]. In response to dilation of the balloon in the rectum, the decrease of pressure in the jejunum and ileum was seen. According to Shafik, this reaction inhibits the transit of the small intestine, allowing the rectum to expel its contents [6]. The continence starts above the rectum. Between the descending and sigmoid colon there is a physiological "colosigmoid sphincter" (CSS) a length of 2.1±0.9 cm. In this zone, the pressure was significantly higher than in the adjacent segments. After a quick inflation of the balloon of large diameter in the descending colon, the decrease of pressure in the CSS was noted. After inflating the same balloon in the sigmoid colon, the pressure in the CSS increases. On the other hand, inflation with a small balloon did not affects the tone of this sphincter. It is clear that the CSS is involved in a passage of large intestinal contents. CSS retains the feces until it reaches a certain volume [7]. Between the rectum and sigma is located the intestinal segment of 2.8±0.9 cm length with the layer of circular muscle thickened in comparison to the segments above and below it [8]. While the pressure in the sigmoid colon increases, this functional rectosigmoid sphincter (RSS) relaxes. In response to increased pressure in the rectum, its tonus rises [9]. Different reactions of RSS to different volume of the balloon were found. After a quick inflation of the balloon in the sigma with 52.1±3.6 ml of liquid, the tone of the RSS increased but the rectal pressure did not change. After the rapid inflation into the balloon of 86±4.1 ml, the RSS relaxed and the balloon was dispelled to the rectum. It was accompanied by an increase of the rectal pressure, and the balloon was expelled [10]. Thus, the RSS with CSS prevent the rapid advance of the large contents of the colon into the rectum. They are the first level of the continence. The rectum is a reservoir, as well as it is involved in the process of defecation by strong contractions [1].
The anal canal is the final section of the digestive tract, which at a manometric study is defined as a zone of higher pressure in comparison to the rectum. Its length ranges from 1.7 cm at birth to 3.6 cm in adults [11,12]. It is located in the center of the pelvic floor muscles, which fan out from it and are attached to the pelvic ring. Each of the two levator ani muscles (LAM) which form a pelvic diaphragm is subdivided into four muscles: pubo-coccygeus, ileo-coccygeus, coccygeus, and puborectalis, which are located on both sides of the median line. These muscles are attached peripherally to the pubic bones, the ischial bones and to the arcus tendineus, as thickened part of the obturator fascia. It is known that muscle fibers of the LAM are intimately connected with the deep portion of the EAS on the side and posterior walls of the anal canal [13, 14]. It is unclear whether the PRM are a component of the LAM or EAS [15]. These muscles are difficult to be differentiated from each other [16]. The vast majority of authors believe that the LAM relaxes during defecation, and this is a basic concept in the pathophysiology of the various diseases of the anorectal area [1,15,16,17].
"Muscles in general have a relatively simple function; they shorten as they contract. In fact, during pelvic floor contraction, the coccyx moves ventrally and cranially" [16]. This muscles are attached to two points. This means that during the LAM contraction, the wall of the anal canal moves in circles towards the periphery, i.e. stretches to the periphery. It is shown that electrical stimulation of the LAM and the puborectal muscles by the needle electrode does not change the pressure in the empty rectum. However, when the balloon of 156.6±34.3 ml is inserted - average pressure in the rectum increases to 64.6±18.7 cm H2O, the need to defecate appears and the balloon is expelled [18]. Since electrical stimulation causes muscle contraction, this suggests that defecation accompanied by a contraction, rather than relaxing of the LAM. Li and Guo showed by use of CT defecography, that the LAM main function is to open the genital hiatus and the anus during defecation [19]. Thus, in the literature there are two opposing views on the role of the LAM during bowel movements: according to some researchers, it relaxing, according to others - it shrinking.
Circular muscle layer of the rectum expands caudally into the anal canal and "forms" the IAS. Circular muscle in the IAS is thicker, than in the rectal wall, and there are septa between muscle bundles. The longitudinal muscles of the rectum extend into the anal canal and end up as thin septa that penetrates into the PRM and EAS. [14,15].
The EAS has three separate muscles bundles – subcutaneous, superficial and deep. The subcutaneous portion of the EAS is located caudal to the IAS, and is attached to the coccyx. The superficial portion surrounds the distal part of the IAS. The deep portion of the EAS is either very small and merges with PRM. Reflex and voluntary contraction of the EAS supports continence for a short time, when a rise in abdominal pressure occurs, during a cough or with positional changes. Partial contraction of the EAS during the passage of flatus observed. This mechanism ensures retention of feces during the exit of gases in the presence of normal anorectal sensitivity [14,15]. The anal resting tone was generated by nerve-induced activity in the IAS (45% of anal resting tone), myogenic tone in the IAS (10%), the EAS (35%) and the anal haemorrhoidal plexus (15%) [20].
The PRM is a muscle loop with two legs are attached to the middle of the inferior pubic rami on both sides. It passes behind the upper part of the anal canal and during contraction pulls it forward. Accordingly, contraction of the PRM results in an acute anorectal angle formation and relaxation (during defecation) causes this angle to become obtuse [21,22]. Based on the physiological studies, it appears that the PRM is the 3-ed sphincter of the anal canal.
In 1877 Gowers found that injection of air into the rectum causes a decrease in pressure in the anal canal [23]. Inflating balloon in the rectum causes a decrease in pressure in the upper part of the anal canal and an increase of the pressure in the lower part. As shown by numerous studies, reducing pressure in the upper part of the anal canal is due to the IAS relaxation, and the increasing pressure in the lower part of the anal canal is due to contraction of the EAS and PRM (rectoanal inhibitory reflex) [24,25,26]. It was found that a pacemaker located in the most gut [25], and that the motor activity of the anorectum is under the control extra rectal autonomous innervation [27].
Methods. In Byelorussian Center of Pediatric surgery 65 children aged from 5 days to 15 years were studied in 1975-1983 for localization of space-occupying lesions and abdominal pain. Twenty three adults patients aged 23-84 years were studied in 1995-2010 in the State Geriatric Center (Israel) in search for the cause of anemia or abdominal pain. In these patients no pathology of anorectal area and the colon was found [28,29].
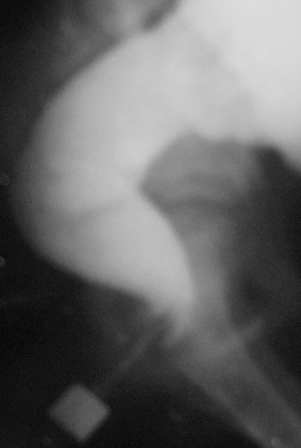
X-ray examination was carried out by a barium enema, which differs from the conventional method of investigating by presence of the radiopaque marker near the anus. Barium was introduced cranially to splenic flexure. On the lateral radiograph of anorectal zone we measured the roentgen negative distance (RND) between barium in the rectum and the marker near the anus on the posterior contour of the tip of the enem a (Figure 1).
A

B
Figure 1. X-ray imaging of the anal canal in the lateral projection (A) and scheme to it (B).
А. A child 11 years. The axis of the anal canal (AC) is shifted forward with respect to the axis of the rectum.
B. The scheme: OK - axis of vertical branch of the rectum; NM - axis of horizontal branch of the rectum; AC - axis of anal canal; P - pubis; PRM – puborectalis muscle, P – pubis, R - radiopaque marker near the anus.
Manometric study carried out with a device consisting of endotracheal tube with diameter of 5.5 cm with a latex cuff. Before the study, the endotracheal tube was lowered into hot water and 3 cm3 of air was introduced into its latex cuff. This tube was connected to the manometer through a three-way crane (Figure 2). Before the study, after introducing 3 cm3 of air into the cuff and switching of the cuff to manometer, the pressure reading was zero. The study was carried out in patient lying on the side. The tube with a deflated cuff was inserted into the rectum. After inflating of 3 ml air in the cuff, it was placed in anal canal and connected to the manometer. The rest pressure measured one minute after the bringing down of the balloon into the anal canal. Then 20 - 50 cm3 of air, depending on the age, was blown rapidly into the rectum through the tube. This provoked the rectoanal inhibitory reflex. In the 10 children barium enema performed while the above-described manometric device was applied. The anal pressure was measured during filling of the rectum by the contrast material (Figure 3).

Figure 2. Scheme of manometric device.
1. Endotracheal tube;
2. Latex cuff, located in the anal canal;
3. Subcutaneous portion of the EAS;
4. IAS;
5. Tonometer;
6. Three-way valve with a syringe.

Figure 3. Implementation of a barium enema through the endotracheal tube of the manometric device.
a) endotracheal tube put into the rectum so that its cuff is at the level of the anal canal.
b) bag with a contrast agent,
c) schedule pressure in the anal canal during barium enema.
Statistical analysis was performed by the method of the Student's t-test. The level of significance was set as P<0.05.
Results. The RND has increased from 1.7 cm at birth to 3.9±0.1 cm in teens and reached up to 4.3 cm in adults. According to the manometric studies [2,11,12,16] its length is equal to the length of the anal canal. In fact, by measuring the RND, we measure the length of the closed anal canal. The measurement results of width of the rectum and length of the anal canal in the patients of different ages are given in the table.
Table. The normal size of the rectum and anal canal in different ages.

In newborn axis of the anal canal coincides with the axis of the rectum (figure 4, A). Over time the upper part of the anal canal shifts forward (figure 4, B). During barium enema, we observed penetration of contrast agent into upper part of the anal canal in front of the enema tip, while the posterior wall tightly pressed to the tip (figure 4, A,B) [30]. Within a few seconds, barium, which had penetrated into the anal canal, returned into the rectum.

A

B
Figure 4. Lateral radiographs of anorectal zone.
Penetration of contrast material in front of the tip of the enema is determined. Posterior wall of the anal canal is pressed against the tip of the enema as a result of contraction of the PRM and EAS (inhibitory reaction).
A. Child aged 4 months. Axis of the rectum and anal canal are the same. Has not yet appeared horizontal displacement of the distal part of the rectum.
B. Patient aged 15 years. The axis of the anal canal is shifted forward from the vertical part of the rectum.
Manometric study was performed in 22 patients. We observed a sudden jump in pressure up to 80-90 mm Hg after introducing of the cuff down into the anal canal (reflex pressure). It is caused by a reflex contraction of the EAS in response to stretching of the anal canal by inflated cuff. Within a 10-20 seconds the pressure decreased and stabilized at the level of 40-50 mm Hg. (43.0 ± 0.8 mm Hg). This basal pressure is determined by the tone of the IAS. When the child felt anxious or when we asked a child to squeeze her buttocks, pressure rose to 80-90 mmHg. It progressively decreased within one minute to the basal level, despite continued efforts of the child. This is a volitional pressure caused by the EAST contraction. After a sharp injection into the rectum of 20 to 50 cm3 of air, the anal canal pressure was reduced to 10-15 mm Hg. Then, it rose during the course of a few seconds to the baseline. This short lived reduction in the anal pressure is determined by relaxation of the IAS and is evidence of the positive rectoanal inhibitory reflex.
In 10 cases the contrast agent was injected into the rectum through an endotracheal tube of manometric device. In the process of the colon filling one to 3 times the penetration of contrast media into the anal canal in front of the enema tip was observed. It lasted a few seconds and then barium disappeared from the anal canal. Appearance of barium in the anal canal is always accompanied by a decrease of the anal pressure by 10-15 mmHg. When barium disappeared from the anal canal, the pressure increased to basal level. Periods of low pressure in the anal canal takes much less time than the periods of normal basal pressure.
Five children defecated during the barium enema. This was accompanied by the anal canal opening to the width equal to the width of the rectum (3.0 - 3.5 cm) (Figure 5).

A

B
Figure 5. Start involuntary defecation with an attempt to strong-willed retention. The anal canal opens to the diameter of the rectum, but almost all of the barium remains in the intestine as result of the subcutaneous portion of the EAS contraction.
Discussion. High pressure in the anal canal (25 - 85 cm H2O) compared with the pressure in the rectum (2-5 cm H2O) is the result of contraction of the IAS, PRM and EAS [30]. Only the IAS of these sphincters has a steady tone [31]. Resting pressure is subject to regular oscillations. They consist of slow waves (amplitude of 5-25 cm H2O) with a frequency of 10-20 oscillations per minute and the slow waves with much larger amplitude (30-100 cm H2O) at three oscillations per minute [32]. These waves come from the IAS as well as electrical recording of the IAC show variations with the same frequencies [33]. In the IAS have been found cells with morphological and immunological phenotypes similar to cells of Cajal, which are believed to be responsible for the generation of electrical activity in the colon and stomach [34]. At the same time, we know that the efferent nerve impulses in the smooth muscle did not initiate and regulate the contraction [35].
Contraction of the muscle fibers is a "work" accompanied by an energy consumption, without its renewal muscle can not continue to contract. Following the contraction inevitably the muscle relaxation must arise, during which the muscle restores its capacity for subsequent contraction. The ability of the IAS to prolonged and continuous contraction can be explained by the fact that the muscle bundles do not contract simultaneously. It is known that the sheaves of smooth muscle fibers anastomosing with each other forming a tightly knit group of fibers, which operate more or less together [35]. Likely that the different groups of smooth muscle fibers in the IAS are at different stages of recovery of the contractile capacity. At any moment an electrical stimulus that excited from the cells Cajal, leads to a contraction of the groups that are ready to contract. By the next wave of electricity, other groups which have fully restored their capacity are stimulated. This continuous process provides a permanent contraction of the IAS. When there is a need to strengthen the fecal retention, extra intestinal nerve centers generate a more strong electric potential. This leads to the contraction not only of the muscle fibers group which is ready to contract, but also, the additional groups that are close to this state. Contraction of the larger number of the muscle groups leads to increased pressure in the anal canal.
The pressure in an empty or relaxed rectum is equal to the intra-abdominal pressure (basal rectal pressure - BRP). During the barium enema periodic penetration of barium into the anal canal in front of the enema tip is accompanied by a decrease an anal pressure. The same radiological picture was observed during defecography. In these cases, the penetration of barium into the anal canal is due to relaxation of the IAS, and the posterior wall of the anal canal moves forward as a result of contraction of the PRM [36]. Relaxation of the IAS appears as response to increase of the rectal pressure above the threshold level [15]. This threshold level pressure which stimulates of the rectoanal inhibitory reflex we called "the first threshold level pressure" (TLP-1). At this time, contraction of the PRM together with the EAS prevents leakage of barium from the rectum. We called the reaction of the IAS, PRM, and EAS in response to increased pressure in the rectum to the threshold level - the inhibitory reaction. Within one minute the rectum adapts to the volume of its content. The rectal pressure decreases to BRP, and the inhibitory reaction is replaced by a reaction of adaptation - contraction of the IAS and relaxation of the PRM and EAS. Musial F. and Crowell MD. showed an adaptive response of the rectum to distention and implied a role for this adaptive response in the determination of rectal sensory thresholds [37]. In this phase the continence achieved by the IAS contraction. In the process of ontogenesis as a result of periodic contraction of the PRM in the first year of life the axis of the anal canal is displaced gradually forward relative to the axis of the rectum. Due to the forward displacement of the rectoanal compound the force of the peristaltic waves, acting on a formed stool, is directed at the horizontal wall of the rectum (figure 6, A). This prevents rectoanal connection from high pressure and thus contributes to continence. Upon admission to the rectum a next portion of the feces, when the pressure in the rectum again rises to the TLP-1, there is a relaxation of the IAS and the contraction of the PRM and EAS (inhibitory reaction). Despite the decrease in tone of the IAS, the anal canal remains closed. When gas or liquid enters into the rectum the pressure is distributed evenly on all walls. Since, the tone of the IAS is reduced, gas or liquid penetrate into the upper part of the anal canal (figure 6, B).

A
B
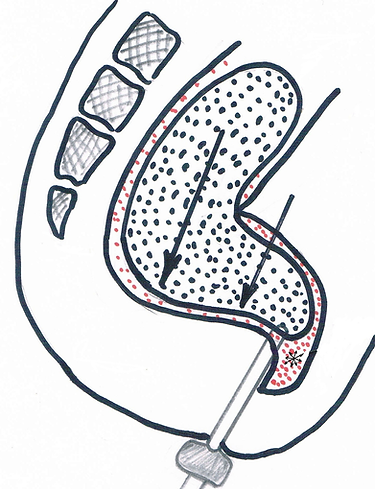
Figure 6. Scheme of the inhibitory reaction and separation of the rectal contents.
А. With the rise of rectal pressure to the threshold level the tone of the IAS decrease, but the stool does not move and anal canal was not seen. The arrows show the vector of fecal pressure.
B. Gas pressure is distributed uniformly in all directions. Therefore, when the IAS tone is reduced, the gas penetrates into the upper part of the anal canal and affects the sensory receptors.
Sensitive elements in the mucosa of this region can reliably detect the presence of gas and liquid [14]. If the situation allows, the person, applying light stress, expels gas through the serried anal canal. In cases where at the moment it is impossible to get rid of gas or in the anal canal liquid feces are present, voluntary contraction of the EAS closes the anal canal and continues until the inhibitory reaction will be replaced by the adaptive reaction. Then, by contraction of the IAS, gas or liquid which penetrated into the upper part of the anal canal, is squeezed back into the rectum. Periodic change of the inhibitory reaction by adaptive reaction and vice versa promotes prolonged retention of feces. During contraction of the IAS, the EAS and PRM restore its contractile capacity, and during contraction of the EAS and PRM, the IAS restores of it ability to contract.
The principal function of the colon include dehydration and storage of ileal content to form feces [38]. Formed portions of feces enter into the rectum from the sigmoid gradually during the day (figure 7).

A

B
Figure 7. The radiographs of the anorectal area of 8 year old child, performed 24 hours after oral administration of a barium suspension (passage).
А. Direct X-ray.
B. Lateral radiograph. Lateral radiograph. During the slow promotion of the feces towards the anal canal they decrease in volume and become more contrast (more dense).
Sleep greatly reduces colonic activity, which immediately increases on awakening. After meals motility rises considerably, perhaps because of cholecystokinin activity, while the extrinsic nervous plexus also has appreciable effect [38]. As a result, in the morning after a meal a large amount of feces quickly enters into the rectum. Rectal distention is perceived as rectal fullness or as a desire to defecate. The amount of the feces, which is the trigger of this perception, depends on the tone of the rectum. The higher the tone of the rectum, the lower the amount of feces needed to cause a desire to defecate, because the receptors of the rectum respond to rectal pressure (urgent pressure). We called the pressure at which there is the urge to defecate, the second threshold level pressure - TLP-2. If the need for defecation combined with the possibility of its implementation should be increased rectal pressure to a certain threshold (defecation pressure). For this purpose, a man in a certain position creates tension of anterior abdominal wall to increase intra-abdominal pressure. This level we call the third threshold level pressure - TLP-3. Thus, the defecation pressure is above the urgent pressure. If in the sense of urge there are no conditions for the rectal emptying, inhibitory reaction arises, which is replaced by the adaptive reaction. The rectum adapts to additional amount of feces, i.e., the tone of its wall decreases and the pressure in the rectum falls below the TLP-2. The next portion of feces, entering into the rectum, again increases the pressure to the TLP-2 and everything is repeated until there will be conditions for defecation.
In 5 children who are not toilet trained the involuntary defecation appeared during a barium enema. This was accompanied by the wide opening of the anal canal to the width equal to the diameter of the rectum. Contraction of the distal part of anal canal around the tip of the enema prevented quick release of a barium. If during defecation the all muscles around the anal canal are relaxed, the expulsion of the liquid barium through the anal canal ought to be a narrow jet. So it happens in some patients with functional constipation [36,39]. In 1983, on the basis of these observations, we concluded that during defecation the wide anal canal is formed as result of the LAM contraction [17]. This hypothesis was confirmed by other researchers [19]. All other muscles of the anorectal area relax during defecation. Deep and superficial part of EAS stretched around the perimeter of the wide anal canal, but the subcutaneous part of the EAS is not involved in this process, as it is located caudal to the IAC and out of the zone of action of the LAM (Fig. 8).

Figure 8. Scheme of the anal canal opening during defecation.
Lateral view: A and B; Sagittal section: C and D.
A and C – before defecation. B and D – during defecation peristaltic wave pushes the feces through the anal canal, which is opened to the width of the rectum as a result of contraction of the LAM. The PRM, IAS, as well as deep (1) and superficial (2) of the EAS, are stretched up to the width of the rectum.
The elastic muscle of subcutaneous portion of EAS has certain resistance. If the stool is soft, the subcutaneous ring of EAS forms a stool with a narrower diameter. Shafik and co-workers have shown that opening of the anal canal during bowel movements is accompanied by peristaltic wave that begins from rectosigmoid junction and continues distally so the feces are expelled from the rectum [40]. The research results of Petros and al "... are consistent with the hypothesis that pelvic striated muscle actively opens the rectal lumen, thereby reducing internal anorectal resistance to expulsion of feces" [41].
Conclusion:
Hypothesis of the continence and defecation
Gastrointestinal tract functions as a single unit, all parts of which are closely linked together. This relationship minimizes the efforts to perform its motor function. For example: the higher the pressure in the rectum, the higher the tone of the rectosigmoid sphincter.
Continence.
-
The continence of stool starts between the descending and sigmoid colon, where functional "сolosigmoid" sphincter is located. Liquid feces linger in front of this sphincter, until they reach a certain volume, because the sphincter does not respond to the pressure which is created by the small amounts of the feces, i.e., it remains closed. At this time, fluid from the feces is absorbed by the intestinal wall. Later more dense and big portion moves into the sigmoid colon.
-
The rectosigmoid sphincter performs a similar function. Some portions of the feces, that have passed through the colosigmoid sphincter, are delayed above the rectosigmoid sphincter. Still moving through the sigmoid colon, they decrease in volume due to absorption of water and are hold over rectosigmoid sphincter. Only when stools reach certain volume they pass into the rectum.
-
This process continues in the rectum. The feces slowly move toward the horizontal portion of the rectum, decreasing in volume and becoming more dense. In some cases, individual portions merge into a single mass. When progress is slow or excess dehydration is present, the stool reaches the final stage in the shape of round and dense aggregations – "sheep feces".
-
In the process of ontogenesis as a result of prolonged contraction of PRM which pulls the upper part of the anal canal forward, distal part of the rectum acquires a horizontal position. It serves as a barrier in the way of the feces, and thereby prevents the penetration of feces into the anal canal.
-
The continuous contraction of the anal canal is provided by the coordinated work of the two types of muscles: the IAS and PRM with EAS. When the next portion of the feces enters into the rectum, and the rectal pressure increases above the threshold level (TLP-1), reflex relaxation of the IAS and contraction of the EAS and PRM (inhibitory reaction) arise. At this time, retention of feces is provided by the contraction of the striated muscle of the EAS and PRM. The rectum adapts to this pressure and relaxes. As a result, the rectal pressure drops below the TRP-1. This leads to a contraction of the IAS and a relaxation of the EAS and PRM (adaptive reaction). In this phase, retention of feces is provided by the contraction of the IAS. When the rectum receives a new bolus of the stool or abdominal and rectal pressure increase above the TLP-1, this again leads to the inhibitory reaction, which is replaced by the adaptive reaction. Multiple repetition of this situation contributes to the long-term fecal retention, because during the relaxation of the muscles their capacity to contraction is recovered. Adaptation reaction lasts much longer than the inhibitory reaction.
-
Most of the time the anal canal is blocked by contraction of the IAC. We hypothesized that many groups of the muscle bundles are in a various stages of recovery of the contractile capacity. At any moment an electrical stimulus that excited by the Cajal cells, leads to a contraction of the group, which is ready to contraction. During the next electric wave, other groups of muscle bundles are contracted, while the previous muscle fibers relaxed for recovery of their contractile ability. All groups of the muscle bundles are contracted at different times in a vicious circle. This can explain the ability of the IAS to provide the continuous continence. If there is a need to enhance the tone of the IAS, extra-intestinal center sends more intense electrical stimulus that causes a contraction of an additional number of the groups "almost ready to contraction". In this case, the tone of each muscle fiber is not changed, but the tone of the IAS rises.
Separation of the rectal contents occurs during the inhibitory reaction. At this time the tone of the IAC is reduced, the solid feces remain in the rectum, and gas or liquid penetrate into the upper part of the anal canal. The sensitive elements in the mucosa of this area can reliably determine the presence of gas or liquid. If the situation allows, the person, applying light tension expels gas through the serried anal canal. In cases where it is impossible to get rid of gas, or in the anal canal is the liquid feces, inhibitory reaction is replaced by an adaptive reaction. Then, gas or liquid, that has penetrated into the upper part of the anal canal, is squeezed back into the rectum as a result of the IAS contraction.
Defecation
When a large amount of feces quickly enters into the rectum, the rectal pressure raises to a higher level – TLP-2. This is perceived as a desire to defecate (urgent pressure). Amount of feces, needed to create urgent pressure in the rectum, depends on the tone of its wall. The higher tone of the rectum, the lower amount of the feces necessary to achieve the TLP-2. If the need for defecation is combined with the opportunity to use toilet, the person tenses to increase the intra-abdominal pressure and the rectal pressure rises to a higher level (TLP-3) (defecation pressure).
Defecation i.e. evacuation of stool from the rectum, is provided by several factors:
a) The normal defecation is possible if the maximum width of the open anal canal fits the thickness of feces formed in the rectum.
b) Feces are expelled from rectum by fast and strong peristaltic wave, which starts from rectosigmoid sphincter, goes through the rectum and continues to the entrance of the anal canal.
c) Simultaneously the wide disclosure of the anal canal for the passage of feces is provided by contraction of the LAM at the level of the deep and superficial parts of the EAS.
d) Subcutaneous part of the EAS relaxes during defecation, but it does not stretch by the LAM contraction. Therefore, the EAS provides some resistance to stool movement. Thus, the soft stool is formatted as a narrow ribbon.
This hypothesis of the continence and defecation can change the conventional understanding of the pathogenesis of anorectal diseases such as chronic constipation, anorectal anomalies, etc. Further research is needed, which may lead to development of new methods of investigation and treatment of these diseases.
References
-
MacCrea GL, Miaskovwski C, Stotts N et al. Pathophysiology of constipation in older adult. World J Gastroenterol 2008 May 7;14(17):2631-8.
-
Meunier P, Mollard P, Jaubert de Beaujeu M. Manometric studies of anorectal disorders in infancy and childhood: an investigation of the physiopathology of continence and defaecation. Br J Surg. 1976 May; 63(5):402-7.
-
Levin MD. Roentgenofunctional studies of feces retention and defecation. Rentgenologia (Moscow) 1983(2): 49-52.
-
Shafik A. Esophago-rectal reflex. Description and clinical significance. Int Surg. 1993 Jan-Mar;78(1):83-5.
-
Shafik A, El-Sibai O. Esophageal and gastric motile response to rectal distension with identification of a recto-esophagogastric reflex. Int J Serg.2000;1(5):373-9.
-
Shafik A. Effect of rectal distension on the small intestine with evidence of a recto-enteric reflex. Hepatogastroenterology.2000 Jul-Aug; 47(34):1030-3.
-
Shafik A, Shafik AA, el-Sibai O, Ahmed I. Colosigmoid junction: a study of its functional activity with identification of a physiologic sphincter and involvement in reflex actions.J Invest Surg. 2003 Jan-Feb;16(1):29-34.
-
Shafik A, Assad S, Doss S. Identification of a sphincter at the sigmoidorectal canal in humans: histomorphologic and morphometric studies.Clin Anat. 2003 Mar;16(2):138-43.
-
Shafik A. The hypertonic rectosigmoid junction: description of a new clinicopathologic entity causing constipation. Surg Laparosc Endosc. 1997 Apr;7(2):116-20.
-
Shafik A, Shafik AA, El Sibai O, Ahmed I, Mostafa RM. Role of the rectosigmoidal junction in fecal continence: concept of the primary continent mechanism. Arch Surg. 2006 Jan;141(1):23-6.
-
Kumar S, Ramadan S, Gupta V, et all. Manometric tests of anorectal function in 90 healthy children: a clinical study from Kuwait. J Pediatr Surg. 2009 Sep;44(9):1786-90.
-
Gruppo Lombardo per lo Studio della Motilita Intestinale. Anorectal manometry with water-perfused catheter in healthy adults with no functional bowel disorders. Colorectal Dis. 2010 Mar;12(3):220-5.
-
Wilson PM. Understanding the pelvic floor. S Afr Med J. 1973. Jul;47(26):1150-67.
-
Coloproctology and pelvic floor. Pathophysiology and management. MM.Henry, M. Swash. Butterworths. 1985.-Moscow, Medicina 1988. p.155-6.
-
Bharucha AE. Pelvic floor: anatomy and function. Neurogastroenterol Motil.2006; 18, 507-19.
-
Raizada V, Mittal RK. Pelvic floor anatomy and applied physiology. Gastrointerol Clin North Am. 2008 Sep;37(3):493-1016.
-
Levin MD, Troyan VV. Anatomy and physiology of anorectal zone. Hypothesis of continence and defecation. Novosti Chirurgii (Vitebsk) 2009; 2: 105-18.
-
Shafik A, El-Sibai O. Effect of pelvic floor muscle contraction on vesical and rectal function with identification of puborectalis-rectovesical inhibitory reflex and levator-rectovesical excitatory reflex. World J Urol.2001 Aug;19(4):278-84.
-
Li D, Guo M. Morphology of the levator ani muscle. Dis Colon Rectum. 2007 Nov;50(11):1831-9.
-
Penninckx F, Lestar B, Kerremans R. The internal anal sphincter: mechanisms of control in maintaining anal continence. Baillieres Clin Gastroenterol 1992;6:193-214.
-
Shorvon PJ, McHugh S, Diamant NE, et al. Defecography in normal volunteers: results and implications. Gut 1989;30:1737-49.
-
Fletcher JG, Busse RF, Riedere SJ, et al. Magnetic resonance imaging of anatomic and dynamic defects of the pelvic floor in defecatory disorders. Am J Gastroenterol 2003;98:399-411.
-
Gowers WR. The autonomic action of the sphincter ani. Proceedings of the Royal Society (London). 1877;26:77-81.
-
Schuster MM, Hendrix TR, Mendeloff AL. The internal anal sphincter response: manometric studies on its normal physiology, neural pathways, and alteration in bowel disorders. J Clin Invest. 1963 Feb; 42:196-207.
-
Meunier P, Mollard P. Control of the internal anal sphincter (manometric study with human subjects). Pflugers Archiv. 1977; 370: 233-9.
-
Rosenberg AJ, Vola AR. A new simplified technique for pediatric anorectal manometry. Pediatrics 1983 Feb; 71(2):240-5.
-
Shepherd JJ, Wright PJ. The response of the internal anal sphincter in man to stimulation of the presacral nerve. Amer J Dig Dis. 1968; 13: 421-7.
-
Misharev OS,Levin MD. Functional and roentgenological studies of the anorectal area in intestinal diseases.Rhirurgiia (Mosk) 1984 Dec; (12):78-82.
-
Levin MD. Roentgenologic anatomy of the colon and rectum in children. Vestn Rentgenol Radiol.1985 Mar-Apr;(2):40-5.
-
Taylor BM, BeartRW, Phillips SF. Longitudinal and radial variation of pressure in the human anal sphincter. Gastroenterol. 1967; 52:1143.
-
Bennett RC, Duthie HL. The functional impotence of the internal sphincter. Brit J Surg.1964; 51:355-7.
-
Haynes WG, Read NW. Anorectal activity in man during rectal infusion of saline: a dynamic assessment of the anal continence mechanism. J Physiology. 1982; 330: 45-56.
-
Halligan S, Bartran CI, Park HJ, Kamm MA. Proctographic featureof anismus. Radiology. 1995 Dec; 197(3):679-82.
-
Shafik A, El Sibai O, Ahmed I. The identification of specialized pacemaking cells in the anal sphincters. Int J Colorectal Dis. 2005 Aug; 9:1-5.
-
Histology. By edition A.W. Ham and D.H. Cormack Eighth Edition. 1979. JB. Lippincoft Company.
-
Nussel D, Genton N,Bozic C. Semiologie radiologique fonctionelle dans la maladie de Hirschprung et dans d’autres formes de dischesie. Ann Radiol. 1976;19(1):111-22.
-
Musial F, Crowell MD. Rectal adaptation to distention: Implications for the determination of perception thresholds. Physiol Behav. 1995 Dec;58(6):1145-8.
-
Irving MH, Catchpole B. ABC of colorectal disease. Anatomy and physiology of the colon, rectum and anus. BMJ.1992 Apr 25;304(6834):1106-8.
-
Levin MD. Functional megacolon in children. Pediatriia (Mosk). 1983 Aug; (8):20-4.
-
Shafik A, Shafik AA, El-Sibai O, Ali YA. Videodefecography: a study of the motile pattern. Surg Radiol Anat. 2003 May 25(2):139-44.
-
Petros P, Swash M, Bush M, Fernandez M, at al. Defecation 1: Testing a hypothesis for pelvic striated muscle action to open the anorectum. Tech Coloproctol. 2012 Dec;16(6):437-43.
